|
|
|
 |
|
|
|
|
For more articles on biology and medicine, see Biology and Medicine categories in index.
|
|
BIOLOGY & MEDICINE
The Case for Adult Stem Cell Research
by Wolfgang Lillge, M.D.
(Full text of article from Winter 2001-2002 21st Century)
|
|
|
|
| What Are Stem Cells, Exactly?
Problems of ‘Therapeutic Cloning’
Whoever Would Cure, Must Use Adult Stem Cells
Human Treatments
For more articles on biology and medicine, check the subject index
|
|
 The question of stem cells is currently the dominant subject in the debate over biotechnology and human genetics: Should we use embryonic stem cells or adult stem cells for future medical therapies? Embryonic stem cells are taken from a developing embryo at the blastocyst stage, destroying the embryo, a developing human life. Adult stem cells, on the other hand, are found in all tissues of the growing human being and, according to latest reports, also have the potential to transform themselves into practically all other cell types, or revert to being stem cells with greater reproductive capacity. Embryonic stem cells have not yet been used for even one therapy, while adult stem cells have already been successfully used in numerous patients, including for cardiac infarction (death of some of the heart tissue). The question of stem cells is currently the dominant subject in the debate over biotechnology and human genetics: Should we use embryonic stem cells or adult stem cells for future medical therapies? Embryonic stem cells are taken from a developing embryo at the blastocyst stage, destroying the embryo, a developing human life. Adult stem cells, on the other hand, are found in all tissues of the growing human being and, according to latest reports, also have the potential to transform themselves into practically all other cell types, or revert to being stem cells with greater reproductive capacity. Embryonic stem cells have not yet been used for even one therapy, while adult stem cells have already been successfully used in numerous patients, including for cardiac infarction (death of some of the heart tissue).
Stem cells are of wide interest for medicine, because they have the potential, under suitable conditions, to develop into almost all of the different types of cells. They should therefore be able to repair damaged or defective tissues (for example, destroyed insulin-producing cells in the pancreas). Many of the so-called degenerative diseases, for which there are as yet no effective therapies, could then be alleviated or healed.
It is remarkable that in the debate–often carried on with little competence–the potential of embryonic stem cells is exaggerated in a one-sided way, while important moral questions and issues of research strategy are passed over in silence. Generally, advocates of research with embryonic stem cells use as their main argument that such research will enable us to cure all of the diseases that are incurable today–cancer, AIDS, Alzheimers, multiple sclerosis, and so forth. Faced with such a prospect, it is supposed to be "acceptable" to "overlook" a few moral problems.
On closer inspection, however, the much extolled vision of the future turns out to be a case of completely empty promises: Given the elementary state of research today, it is by no means yet foreseeable, whether even one of the hoped-for treatments can be realized. Basically, such promised cures are a deliberate deception, for behind the mirage of a coming medical wonderland, promoted by interested parties, completely other research objectives will be pursued that are to be kept out of public discussion as much as possible.
Perfect candor should rule in stem cell research. This requires that the scientist himself clearly establish the moral limits of his activity and declare what the consequences of research with embryonic stem cells really are. In the process, no one can escape the fact that, should one wish to use embryonic stem cells for "therapeutic purposes," the very techniques will be developed that will also be used for the cloning of human beings, the making of human-animal hybrids, the manipulation of germ lines, and the like–thus for everything other than therapeutic purposes. Any coverup or hypocrisy in this matter will very quickly reflect upon the research as a whole.
What Are Stem Cells, Exactly?
It is appropriate here to sketch the characteristics of stem cells, and the overthrow of some dogmas of developmental biology. Broadly speaking, a stem cell is one that–in the course of cell division and increase in the numbers of cells–is able to reproduce itself and also mature into various specialized types of cells. The stem cell with the greatest potential (totipotential) is the fertilized egg cell, which is capable of developing into a complete organism.
According to the usual–but actually very doubtful–explanation, the fertilized egg cell has totipotential up to the stage of division into eight cells, and in later stages the cells retain only "pluripotential." That is, they can form many different types of tissues, but not the complete organism. Embryonic stem cells–that is, those 50 cells within a blastocyst, which then continue to develop into the embryo proper–have this pluripotential. In the course of further specialization, stem cells of individual tissues are formed, such as that of the bone marrow, from which all the other kinds of blood cells develop.
Behind this description lies the conception that a linear process of differentiation is played out, in the development of the individual, toward increasingly "mature," specialized cells in the individual tissues, from totipotentiality to tissue specificity. This process is supposed to run only forward, but never backward. That is, as soon as a cell has reached a certain degree of "maturity," the way back to earlier stages of development is closed off. So it is evident that a stem cell’s capacity to perform is increasingly limited to specific functions, and it loses, correspondingly, the manifold capabilities still present in earlier developmental stages.
According to latest reports, however, this dogma of developmental biology does not hold. Evidently, tissue-specific stem cells have the ability–as has been impressively demonstrated in experiments with animals–to "transdifferentiate" themselves when in a different environment–that is, to take on the cell functions of the new tissue. Thus, neuronal stem cells of mice have transformed themselves into blood stem cells and produced blood cells. Indeed, there are indications of another capability of adult stem cells: Apparently they have the potential to be "reprogrammed." Not only can they adjust to the specific conditions of a new tissue environment, but they can even assume more generalized, earlier levels of development, so that it even appears possible that they become totipotent again.
|
|
|
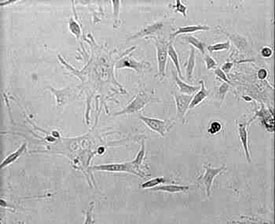 Laboratory Virola in Ukraine has demonstrated that bone marrow stromal cells in culture are pluripotent–that is, they are able to differentiate into cells of liver, bone, fat, cartilage, and so on. Researchers at this laboratory have developed techniques to differentiate in vitro mouse bone marrow stromal cells into different types of neuronal and glial cells. The laboratory is seeking funds to develop similar methods for human bone marrow stromal cells. Laboratory Virola in Ukraine has demonstrated that bone marrow stromal cells in culture are pluripotent–that is, they are able to differentiate into cells of liver, bone, fat, cartilage, and so on. Researchers at this laboratory have developed techniques to differentiate in vitro mouse bone marrow stromal cells into different types of neuronal and glial cells. The laboratory is seeking funds to develop similar methods for human bone marrow stromal cells. |
|
|
Laboratory Virola |
|
|
|
|
Problems of ‘Therapeutic Cloning’
Until now, talk of a possible source of human replacement tissue has centered on embryonic stem cells, the production of which has been extremely controversial. They are a typical product of "consuming embryonic research," so called, because in obtaining them from a human embryo produced by artificial fertilization in vitro, the embryo is destroyed.
The most important research technique for which such embryos are obtained is "therapeutic cloning." In principle, a human egg cell is denucleated, that is, the DNA is removed, and in its place is put the nucleus of a somatic (body) cell. The egg cell is stimulated with a short electrical pulse, and it then develops into the blastocyst, from which stem cells can be removed. These are identical with those of the donor of the somatic cell nucleus.
Normally it goes unmentioned, that it is only a small step from this so-called "therapeutic cloning" (because, it is claimed, in this way a therapy for diseases can be developed) to what is called "reproductive cloning." The only difference is that the development of the embryo is not interrupted in the early blastocyst stage; instead the embryo is implanted in a uterus and a complete organism develops–an exact genetic copy of the donor. "Dolly," the first cloned sheep, was produced by this method, and here is the basis for the widespread fear that the same method that is used for "therapeutic cloning" can also be used for the selective breeding of humans.
In addition to the obvious moral consideration, there are still other serious disadvantages that make this path to the development of human "replacement parts" appear to be untenable.
The danger of tumors. So far there has been no solution to the problem of developing in the laboratory an unmistakable identifier for stem cells that can distinguish them unequivocally from cancer cells. For this reason, it is also not possible to produce sufficiently pure cell cultures from stem cells. So far, with embryonic mouse stem cells, a purity of only 80 percent has been achieved. That is in no way sufficient for cell transplantation as a human therapy. In a cell culture for therapeutic purposes, there must not be a single undifferentiated cell, since it can lead to unregulated growth, in this case to the formation of teratomas, a cancerous tumor derived from the germ layers. This problem would not be expected with adult stem cells, because of their greater differentiation.
Genetic instability. Only recently a further problem has emerged. Fundamental doubt of the suitability of embryonic stem cells for transplantation has come to the surface because of the genetic instability of cloned cells.
Cloned animals like Dolly give the outward appearance of full health, but the probability of their having numerous genetic defects is very high. Moreover, the entire cloning procedure is extremely ineffective. Most cloned animals die before birth, and of those born alive, not even half survive for three weeks. In the best case, there is a success rate of 3 to 4 percent.
One of the reasons for this high failure rate has now been discovered by the German scientist Rudolf Jaenisch at the Institute for Biomedical Research at the Massachusetts Institute of Technology, and his colleague, Ryuzo Yanagimachi. Their conception is that in cloning–that is, when the nucleus of a somatic cell is inserted into a denucleated egg cell–the reprogramming of the genes does not proceed properly, so that not all of the genes that are necessary to the early phase of embryonic development, are activated. Even when cloned animals survive at all, probably every clone would have subtle genetic abnormalities that would frequently become noticeable only later in life.
Jaenisch performed his experiments with mice that had been cloned using embryonic stem cells in place of the somatic cells, which produces better results. But to his surprise, the reprogramming of the inserted genetic material by the embryonic cells proceeded in a very unregulated way. There were no two clones in which the same pattern of gene activation was found, and Jaenisch is convinced that the use of embryonic stem cells was clearly responsible.
What consequences follow from this for the therapeutic use of human embryonic stem cells–consequences that will in fact be multiplied through cloning–are not yet foreseeable.
|
|
|
|
|
|
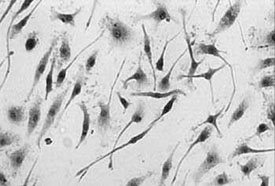 Neuroblasts differentiated from bone marrow stromal cells by Laboratory Virola. Neuroblasts differentiated from bone marrow stromal cells by Laboratory Virola. |
|
|
Laboratory Virola |
|
|
|
|
Whoever Would Cure, Must Use Adult Stem Cells
It has been known for about 30 years that stem cells are present in the tissue of the adult, but it was assumed that they could only form cells of a particular tissue. That is, reprogramming them was considered impossible. In recent years, however, pluripotent stem cells were discovered in various human tissues–in the spinal cord, in the brain, in the mesenchyme (connective tissue) of various organs, and in the blood of the umbilical cord. These pluripotent stem cells are capable of forming several cell types–principally blood, muscle, and nerve cells. It has been possible to recognize, select, and develop them to the point that they form mature cell types with the help of growth factors and regulating proteins.
This shows that in tissues of the body, adult stem cells possess a much greater potential for differentiation than previously assumed. This knowledge must be brought into the public consciousness with all possible emphasis. If stem cell research were really only meant for therapeutic uses, which it most obviously should be, adult stem cells would promise a very productive research field–and beyond that, a possibility, without moral objection, to discover fundamentals of the dynamics of tissue differentiation.
It has become clear from transplantation experiments with animals, that stem cells of a particular tissue can develop into cells of a completely different kind. Thus, bone marrow stem cells have been induced to become brain cells, but also liver cells.
Adult stem cells obviously have a universal program for division that is common to all the kinds of tissue stem cells, and makes them mutually interchangeable. This was discovered by Alexei Terskikh at Stanford University School of Medicine in California. He was able to prove that adult stem cells of blood-forming tissues, and of the brain, activate the same genes, in order to preserve their status as stem cells.
In May 2001, a further, spectacular experiment was reported, which was carried out on mice by scientists at Yale University. The researchers obtained stem cells from the bone marrow of male mice, and injected it into females whose own marrow had been destroyed by radioactive irradiation. Eleven months later, the male stem cells (identifiable through the male Y-chromosome) were found not only in the females’ bone marrow, but also in their blood, and in their gut, lung, and skin tissues.
If these observations are correct and are confirmed by other teams of scientists, science should concentrate on research with adult stem cells and renounce further experiments with the embryonic.
Human Treatments
Moreover, very promising treatments of serious diseases with adult stem cells have already been tried. The special advantage is that there are no rejection reactions, because the cells are from the same body.
Of longer standing is treatment with bone marrow stem cells. The treatment comes into play when, for example, a patient has lost his or her blood-forming tissue through radiation or high-dose chemotherapy. Previously removed bone marrow stem cells are then retransplanted, and are able to resume the formation of blood cells.
In 2001, however, a team of doctors at the Duesseldorf University Clinic carried out a treatment of very far-reaching consequences. For the first time, they treated a cardiac infarct patient with stem cells from his own body. The cardiologist, Prof. Bodo Eckehard Strauer, is sure that the stem cells from the patient’s bone marrow, after injection into the infarct zone, autonomously converted to heart muscle. The functioning of the severely damaged heart clearly improved within a few weeks.
Four days after the infarction, the doctors took bone marrow from the patient’s pelvis using local anesthesia. The stem cells in the marrow were concentrated outside of the body and implanted in the infarct area the next day with a special technique via a coronary artery. However, the doctors could not yet take cardiac tissue to prove definitively that the implanted blood stem cells had converted to heart muscle cells. But, according to Strauer, there is no other way to explain the marked improvement in the patient’s condition. After this first successful operation, six more patients have already been treated with their own stem cells, with similarly positive results.
There are also reports of successful treatments with adult stem cells in cases of Crohn’s disease (a chronic infection of the gut), thalassemia (a blood disease), and a rare skin disease. And–despite the fact that basic research with adult stem cells is in its earliest beginnings and is in no way being promoted with urgency–there have been a growing number of reports lately of experiments with animals, from which it emerges that adult stem cells can successfully transform themselves into differentiated cells of organs of many kinds.
In contrast, reports of successful conversions of embryonic stem cells are very infrequent and cautious. Thus, we find in Science of Dec. 1, 2000 (Vol. 290, pp. 1672-1674): "In contrast, the human embryonic stem cells and fetal germ cells that made headlines in November 1998 because they can, in theory, develop into any cell type have so far produced relatively modest results. Only a few papers and meeting reports have emerged from the handful of labs that work with human pluripotent cells. . . . The work suggests that it will not be simple to produce the pure populations of certain cell types that would be required for safe and reliable cell therapies. . . ."
This is the restrained language used by established science to describe a truly disastrous set of results.
There are, of course, still substantial problems to be overcome, even with adult stem cells: They are relatively rare, and are hard to find with the techniques used so far. They are also not very easy to culture outside of the body. It was therefore an important advance that Australian researchers of the Walter and Eliza Hall Institute of Medical Research have now found a way to isolate nerve stem cells with "extreme purity" from the brains of mice. In Nature of August 16, 2001 (Vol. 412, pp. 736-739), they reported obtaining a culture of 80 percent purity, compared to a previous rate of 5 percent at best.
It is now urgently necessary to tackle the research in precisely this direction, in order to find out the exact conditions under which the differentiation of stem cells comes about and how, in detail, it proceeds. Only by this morally unassailable route will it be possible to develop new therapies for serious, heretofore incurable diseases, and beyond that, to improve our understanding of the development of life itself.
Wolfgang Lillge is the Editor-in-Chief of the German-language Fusion magazine. His article appeared in the Sept.-October 2001 issue of Fusion, and was translated into English by David Cherry.
|
|
|
|
|
|
|
|